Leprosy: The Failed Eradication
Leprosy continues to resist being wiped out in India because the battle against it was called a victory too soon
 Madhavankutty Pillai
Madhavankutty Pillai
 Madhavankutty Pillai
Madhavankutty Pillai
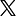 |
31 Jan, 2019
|
31 Jan, 2019

IN 2009, RESEARCHERS FOUND the earliest presence of leprosy in the India. It was roughly 4,000 years ago that a middle-aged man, who now goes by the name of ‘Individual 1997-1’, in Balathal, Rajasthan (then a settlement of the Indus Valley Civilisation) contracted the disease and became prey to the deformities that it causes. His skeletal remains bore, according to the study’s paper published in PlosOne, ‘pathological changes in the rhinomaxillary region, degenerative joint disease, infectious involvement of the tibia (periostitis), and injury to the peripheral skeleton.’
Leprosy is somewhat easy to deduce from such remains because of how it eats into the bone. For instance, Individual 1997-1 showed rhinomaxillary syndrome, which details how particular areas of the nose degenerate, including ‘destruction of the nasal spine’. About his lifestyle, the paper has a hint. In Balathal, people lived in ‘stone or mud-brick houses, made wheel thrown pottery, copper implements, and practiced dry field agriculture focused on barley (Hordeum vulgare) and wheat (Triticum spp.).’ Not a very plush life, but, for the times, not bad either; it was also urbanised, which might well have been responsible for the disease finding a foothold in India.
It might even have spread to the rest of the world from here. A press release of the study had this to say: ‘A report on genomics of Mycobacterium [the bacteria responsible for leprosy] published in the magazine Science by Monot and colleagues in 2005, indicated the disease may have originated in Africa during the Late Pleistocene and that M. leprae spread out of Africa sometime after 40,000 years ago, when human population densities were small. A counter hypothesis was proposed in the same volume of Science by Pinhasi and colleagues suggesting that the same data could be interpreted as evidence for a Late Holocene migration of the disease out of India after the development of large urban centers… The presence of leprosy in India toward the end of this period indicates that M. leprae existed in South Asia at least 4000 years ago. This suggests that there may be some validity to Pinhasi and colleagues hypothesis that the disease spread between Africa and Asia during a period of incipient urbanization, increasing population density, and regular inter- continental trade networks.’
About 500 years later, once the Vedic nomads had arrived in India, in a couple of hymns in the Atharva Veda, they noted a disease called kushta with symptoms of the disease. The Balathal discovery lent further credence to ‘kushta’ being leprosy. It is alluded to frequently in later historical Indian texts. The Buddha was a very inclusive sort of person, but the Vinaya Pitaka, the canon on discipline in his Order, says lepers are not to be admitted. Leprosy has ancient roots in India and so also its stigma. And since the time of its first appearance four millennia ago, its stranglehold on India steadily increased until there were millions of leper outcastes. All that was set to change as the new millennium began.
In 2005, the Government announced that leprosy, thanks to an ambitious drive marked by nationwide house-to-house surveys for early detection, had been eliminated. The definition of elimination was less than one case per 10,000 of the population. In 1983, the prevalence had been as high as 57.8 per 10,000. By 1991, it had been brought down to 25 per 10,000, which was still more than 2 million cases in absolute numbers. But the 1990s saw spectacular success. By December 31st, 2005, it was just 0.95 per 10,000, or a little over 100,000 cases. It was thought that complete eradication would only be a matter of time.
A decade-and-a-half later, leprosy remains more or less where it was in 2005 with the numbers plateauing and sometimes even increasing a little. A paper published last March in the Indian Dermatology Online Journal, said: ‘…the fact remains that India continues to account for 60% of new cases reported globally each year and is among the 22 “global priority countries” that contribute 95% of world numbers of leprosy warranting a sustained effort to bring the numbers down. In the year 2007, new cases detected in India were 137,685, and nine years later in 2016, the number remained almost the same at 135,485, a significant increase over the 127,326 new cases detected in 2015. This increase in new cases is attributed by NLEP (National Leprosy Eradication Programme) to their recent strategy of innovative Leprosy Case Detection Campaign (LCDC), which resulted in the detection of 34 000 new cases in 2016 from highly endemic pockets, which accounted for 25% of annual new cases.’ The numbers could even be higher. A survey done by the Indian Council of Medical Research between 2008 and 2011 said there might be 250,000 cases in the country. It was a number that Union Health Minister JP Nadda cited in a 2016 Indian Express op-ed piece. In 2018, Nadda said that the country would be free of leprosy by this year. But latest figures from the National Leprosy Eradication Programme upto March 2018 still show a little under 100,000 cases officially. Just last week, Dr Poonam Khetrapal Singh, WHO regional director for South-East Asia, had said in a statement, “Though the number of leprosy cases has steadily declined worldwide, an estimated 200,000 cases continue to be reported every year, with India accounting for more than half.” Some media reports even term it a ‘comeback’.
Oommen C Kurian, a researcher at the Observer Research Foundation (ORF) who is soon coming out with a research report on the state of leprosy in India, says that the disease is not making a comeback because it never went anywhere. “The elimination target of 1 per 10,000 population was imposed on us by World Health Organisation. It was an unscientific target. The idea was to have a leprosy prevalence of less than 1 per 10,000 by 2000. India failed to achieve it. So there was huge pressure on countries like India, which had a very big proportion of the patient community, to perform,” he says. As against elimination, which means bringing the number below 1 per 10,000, eradication is to completely remove it from the community. The fact that India had officially achieved elimination ironically became a deterrence to its eradication.
As of March 2018, there were under 100,000 cases officially and it is clear the ailment still persists
Because leprosy was considered eliminated, it was removed from the list of public health concerns with a vertical programme of its own and dedicated resources. It was instead integrated into the main healthcare delivery system. “Till 2005, we had active case detection. People from the health department would come to your house and check if you have leprosy. Post-elimination, we shifted to passive detection. If somebody with leprosy comes to the hospital or healthcare delivery centre, then you will count them in, otherwise you don’t. We diverted the resources from the leprosy programmes to other programmes. It is a self-fulfilling kind of thing—you don’t have resources to find cases, you are not actually doing active detection, so the official numbers will actually remain where they are. But those numbers are unfortunately not an indication of the actual case-load in the community. That has happened for almost a decade,” says Kurian.
A few years ago, the Government realised that it had an issue. And so surveillance initiatives, especially in endemic areas, have again been strengthened. When that happened, they finally began to record cases that had always existed. “We are detecting more because the system has become more active,” he says.
“It is a disease of poverty. The number of patients who are the most marginalised among the poor, adivasis, is shooting up,” says Oommen C Kurian, researcher at the Observer Research Foundation
But Kurian finds a more worrying phenomenon. His analysis details how there was a radical increase in leprosy cases among tribals. The ORF research paper notes, ‘A distinct trend that should worry every health policymaker in the country is that Leprosy is becoming even more of a disease of most marginalized and underserved populations in far-flung areas. We do have some data on the prevalence of Leprosy amongst the Dalits (Scheduled Castes) and Adivasis (Scheduled Tribes) who, according to Census 2011, constitute 16.6% and 8.6% of the Indian population, respectively. However…(in) the percentage of new Leprosy cases in India, patients belonging to these two communities constitute 37.6%—much more than their proportion in the Indian population—and their proportion is increasing. A look at disaggregated data shows that while the proportion of Dalits within new Leprosy cases has stagnated between 18-19%, the overall rise is almost exclusively because of the rise in the proportion of Adivasis within new Leprosy cases over the last decade… From 13.3% in 2009, it has increased to an alarming 18.8%, and given that Adivasis are only 8.6% of the Indian population, it is a cause for major concern.’
Kurian adds, “It is a disease of poverty, everybody knows it. Now the number of patients who are the most marginalised among the poor, Adivasis, is shooting up.” However, it is possible that this might not be a bad thing because it could indicate that the healthcare system is now reaching them. These cases might be coming into the light instead of never being reported at all. Likewise, he says, there is also the phenomenon of the number and proportion of districts that have a prevalence of more than 1 per 10,000 increasing every year. “But you cannot be alarmist and say it is coming back. It can also be that in certain pockets, the health system is reaching populations it never reached before,” he says. This, however, is very difficult to confirm one way or other, given the patchy data.
“The vertical programme should not have been stopped so early. It should have gone on for a longer time for real eradication,” says Utpal Sengupta researcher, Leprosy Mission Trust of India
UTPAL SENGUPTA, who works at the Stanley Browne Laboratory, Leprosy Mission Trust of India, posits another reason why the Government is finding it so difficult to eradicate leprosy completely. Last year, he came out with a paper titled ‘Elimination of leprosy in India: An analysis’ in the Indian Journal of Dermatology, Venereology and Leprology. It too holds the haste with which elimination was announced in 2005 and the resultant integration of leprosy control programme into the general health services responsible for the disease’s persistence, with annual new case detections making up for those that get cured. His paper said, ‘…between the years 2005 to 2015, both prevalence rate and annual new case detection rate remained in a plateau phase and the latter always exceeded the values of the former. This clearly indicates that although the number of cases as determined by prevalence rate has drastically gone down, the active transmission of infection has remained unchanged, as revealed by a steady level of annual new case detection rate.’
Sengupta says one of the reasons for new cases is that the disease can have a long incubation period, ranging from a few weeks to three decades, and this was not factored in when elimination was announced in 2005. Patients didn’t know they had the disease and even when they saw the first signs, whether because of ignorance or the stigma attached to it, they wouldn’t self-report. Earlier, during house-to-house surveys, the disease was diagnosed and reported early.
“There is a lot of stigma still attached to it. And hence whosoever has leprosy doesn’t initially go to a physician. It has to be surveyed, where picking up is done very early. Now, the Government has initiated a Leprosy Case Detection Campaign. They are taking index cases and looking at the contacts too. They have started doing this throughout the country. Once you go for surveys, you get more cases. So, they are getting more new cases. Annual new case detection rates have gone up,” says Sengupta. He thinks rigorous surveillance was necessary for up to a decade even after the 2005 elimination so that such cases would have come to light as soon as the disease incubated.
“I thought that every community and caste has an association. Why not for leprosy patients? Leprosy is our caste,” says Vagavathali Narsappa , president of the Association of People Affected by Leprosy
One simple route for the disease to be eradicated is if the country’s standard of living and health and hygiene improves. Leprosy has an inverse correlation with them. This was how it gradually disappeared in the West after the Industrial Revolution. But in India, that level of development is still far away. Early detection before deformities set in therefore becomes crucial.
Sengupta says, “Until and unless you detect leprosy very early and treat it, it won’t be eradicated. The vertical programme should not have been stopped so early. It should have gone on for a longer time for real eradication.”
One of the fallouts of the 2005 decision to integrate leprosy into general health services was that the funds needed to rehabilitate patients began to dry up. Vagavathali Narsappa, president of the Association of People Affected by Leprosy, remembers being first gladdened on hearing that leprosy was about to be eliminated and then wondering, as a patient with disabilities—he cannot use either of his hands—how he and others like him would survive without support from the Government and NGOs. He had experienced first-hand the stigma of leprosy. In 1977, as a nine-year-old living in a village in Karnataka, the telltale signs of the disease began to appear on him. Villagers told his parents that they would ostracise the family if the boy lived with them. His father left him in a hospital in Nizamabad and never returned to take him back. After his treatment and discharge, he had nowhere to go, until a good samaritan brought him to a rehabilitation home in Hyderabad. He received an education there, but when he went to take a public exam at a centre in his seventh standard, they wouldn’t allow him inside. “I was told to sit out on the ground and the paper was thrown at me from above,” he says.
But Narsappa made a life for himself. He continued working at the rehabilitaton home for 15 years, moving to another NGO after that and also marrying a co-worker with whom he had two daughters. By the beginning of the 2000s, the NGO’s director was repeatedly saying that leprosy was going to be eliminated soon and funding would end.“In 2005, elimination was announced on paper. I thought I was handicapped and needed assistance. Who would give it once the funding was removed? What do we do? I thought every community and caste has an association. Why not for leprosy patients? Leprosy is our caste,” he says. Narasappa formed such an association and through rallies, dharnas, petitions in court, etcetera, has been instrumental in getting governments to provide relief and support to leprosy patients.
“There has been no difference in stigma over the years. There is immediate social death of the patient on realising that he has got the disease,” he says. The problem is not leprosy itself, Narasappa says, but the disability that comes from it. “To counter that, early detection, early treatment is necessary. There is no stigma without deformity.” When elimination was announced, it was this early detection that took a back seat. “In 2005, after the integration, there was neglect. Practically, elimination has not happened. It was a forced elimination. They stopped working on leprosy,” he says.












More Columns
Why I Don’t Look Back in Anger Boria Majumdar
The Playful Past Rati Girish
“The day you say Modi is 'satisfied’, you can say you are paying homage to him” Open