A MATTER OF LIFE
The Unbearable Weightiness of Being
An underactive thyroid gland does not condemn you for life
 Dr Ambrish Mithal
Dr Ambrish Mithal
 Dr Ambrish Mithal
08 Feb, 2017
Dr Ambrish Mithal
08 Feb, 2017
SINCE JANUARY was Thyroid Awareness month, let’s use this opportunity to dispel myths about the most common thyroid disorder, hypothyroidism, which results from an underactive thyroid. Three decades ago, when I was cutting my teeth in endocrinology, iodine deficiency-related hypothyroidism, thyroid enlargement, and mental retardation were some of the most serious public health problems in India. Fortunately, iodine deficiency has been virtually eradicated with the implementation of universal salt iodation. Presently the most common cause of hypothyroidism in India, as in the West, is autoimmunity.
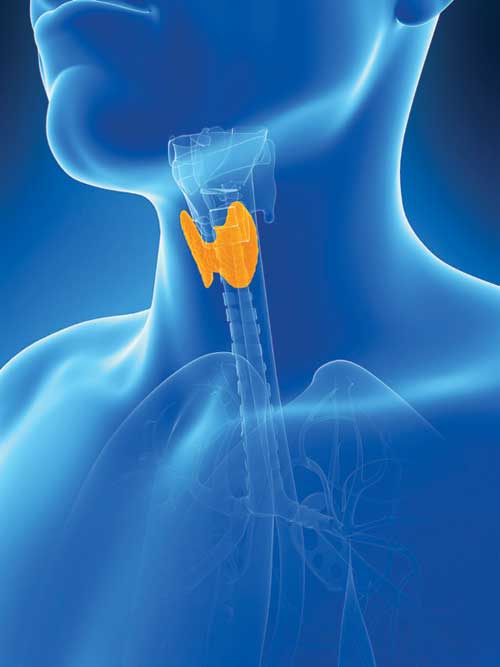
The thyroid gland is a classic example of an endocrine (ductless) gland. By secreting hormones into the blood, endocrine glands are able to deliver their impact on the body distant from their source of origin. The thyroid is a butterfly shaped gland, barely 5 cm in size. Situated in front of the neck, straddling our windpipe, it produces the hormones T4 and T3, which have actions on virtually every part of our body. It is the key regulator of our metabolism and has a profound impact on body temperature. Deficiency of thyroid hormone (hypothyroidism) can lead to dullness, impaired memory, lethargy, dry skin and hair, puffiness, low pulse rate, constipation, menstrual irregularities and weight gain among others. Symptoms are often nonspecific and creep on insidiously, unrecognised.
In common parlance, hypothyroidism is referred to as ‘the disease where one puts on weight’. A diagnosis of hypothyroidism sometimes triggers a sense of relief rather than dismay: ‘I’ve discovered why I was putting on weight’. Unfortunately, most often this is not the case. Mild hypothyroidism is not associated with significant weight gain. Even severe hypothyroidism usually causes a weight gain of only 2-4 kg.
Another frequently asked question relates to diet restrictions for thyroid patients. The internet is full of information about foods that harm the thyroid: cabbage, broccoli, cauliflower, and others. These vegetables may contain goiter-producing substances (goitrogens) which can impact the thyroid adversely. Fortunately, their impact is negligible in iodine sufficient populations. The possible exception is soya bean and its products, which, if taken in excess, could interfere with thyroid treatment. In essence, contrary to popular belief, hypothyroidism is not a lifestyle disease and is not significantly impacted by Indian diets. All the information that you read about diet and the thyroid is therefore to be taken with a pinch of (iodised) salt.
Who should be tested for thyroid disease? The high prevalence suggests that all should be screened, but experts don’t consider this feasible or cost effective. Testing newborn babies should be made mandatory, because hypothyroidism can cause mental retardation which is preventable by timely initiation of treatment. Another important group to be tested is pregnant women, since a low maternal level of thyroid hormone can impact foetal brain development in the first trimester. Treating even minor degrees of hypothyroidism at this stage is critical. Women who have difficulty in conceiving or those with irregular menstrual periods are also candidates for testing, as are children who are lagging in growth. Some suggest that all women above the age of 60 should be tested, in light of the high prevalence in this group. Tests to diagnose hypothyroidism include blood level of thyroid hormone—T4 (thyroxine) and TSH (thyroid stimulating hormone). TSH is secreted by the pituitary gland—an increase in TSH is the most sensitive marker of thyroid function. Not everyone with abnormal thyroid tests needs treatment, in particular those with TSH values that are marginally elevated (between 5 and 10). Many such patients receive unnecessary treatment with little benefit.
If diagnosed with hypothyroidism, you are not condemned for life. It can mean, however, that you have to pop a thyroxine pill for the rest of your days. The good news is that virtually all the effects of hypothyroidism are reversible. There is hardly any side effect if thyroxine is given in proper doses for the right patient. With the right professional guidance, hypothyroidism is easily manageable. Don’t give up your medicine (unless so advised by your doctor) and you will lead a healthy, normal life. Gone are the days when sheep thyroids were minced and injected into humans to treat hypothyroidism. Thyroxine has been in use for more than a hundred years, so be comfortable with it.
About The Author
Dr Ambrish Mithal is Chairman, Endocrinology and Diabetes, Max Healthcare

More Columns
Travellers on Trial Bhavya Dore
Sahir’s Legacy Kaveree Bamzai
The Devi Mystique Bibek Debroy